Chronic Pain and the Biopsychosocial Model - A More Complete Way to Understand Pain
By Katherine Reardon, DPT
If you have been living with pain for months — or even years — you have probably heard something like: "Everything looks normal on your imaging," or "You may just have to learn to live with it." For many people dealing with chronic pain, those words land like a dead end. They do not explain why the pain is still there, and they certainly do not point a way forward.
Modern pain science tells a different story.
Pain — especially when it persists — is rarely just a tissue problem. Chronic pain is best understood through what researchers and clinicians call the biopsychosocial model: an evidence-based framework that looks at the whole person, not just the painful body part. Understanding this model can be one of the most empowering steps toward lasting relief.
What Is Chronic Pain?
Pain is generally considered chronic when it persists longer than three months. At that point, something important shifts: pain often becomes less about ongoing tissue damage and more about how the nervous system is processing and interpreting signals.
This does not mean the pain is "all in your head." It means the body and brain are working together in a pattern that keeps pain signals amplified — even after tissues have healed. The pain is real. The experience is real. But the driver is no longer primarily structural.
The Biopsychosocial Model: What It Means and Why It Matters
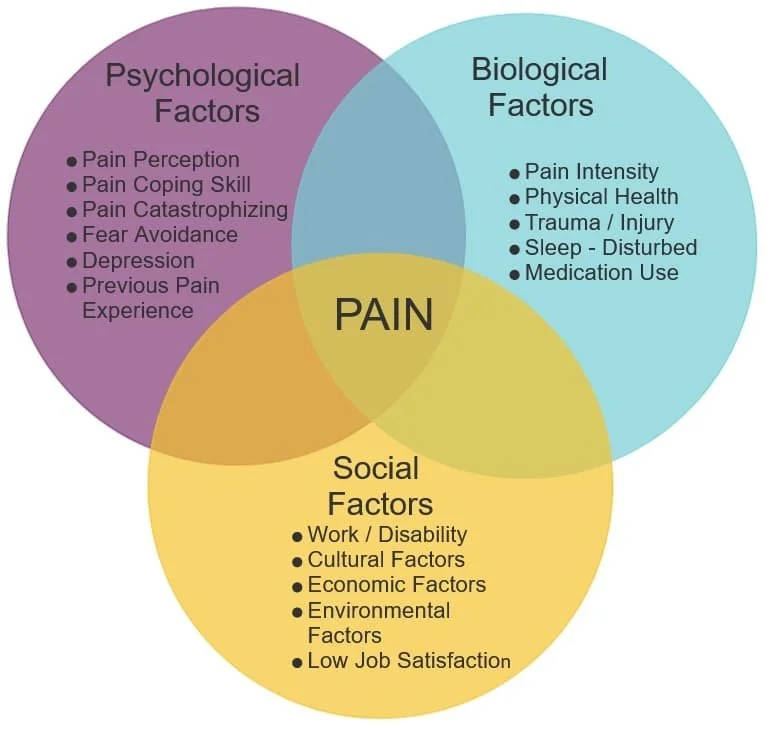
The biopsychosocial model recognizes that pain is shaped by three interconnected systems working simultaneously. No single factor tells the whole story.
1. Biological Factors — The Body
Physical contributors to chronic pain include:
Joint stiffness or reduced mobility
Muscle weakness or deconditioning
Past injuries or surgeries
Nervous system sensitization
Inflammation
Altered movement patterns
In chronic pain, tissues are often less damaged than they feel. Over time, the nervous system can become overprotective — amplifying pain signals in response to movement, stress, or even anticipation of activity, even when no new injury is occurring.
2. Psychological Factors — The Brain and Mind
Psychological factors do not mean pain is imagined. They reflect how the brain interprets and weighs incoming signals from the body.
Common psychological contributors include:
Fear of movement ("If I move, I will make it worse")
Anxiety or chronic stress
Prior pain experiences that shaped expectations
Poor or disrupted sleep
Feelings of helplessness or discouragement about recovery
Research consistently shows that fear of movement, stress, and sleep disruption can heighten pain sensitivity and slow recovery — independent of any structural finding on imaging.
3. Social Factors — Life Context
Pain does not exist in a vacuum. The circumstances of daily life play a powerful and often underestimated role:
Work demands or prolonged sedentary positions
Family responsibilities and caregiving stress
Limited social support or sense of isolation
Financial pressure
Activity restrictions that reduce enjoyment, purpose, or identity
When pain limits daily activities, it tends to create a reinforcing cycle: reduced movement leads to further stiffness and weakness, which feeds back into more pain and more avoidance.
Key Takeaway: The biopsychosocial model is not an alternative to treating the body — it is a more complete framework for understanding why pain persists and what it actually takes to address it.
Why a Whole-Person Approach Leads to Better Outcomes
Traditional pain treatment often focuses exclusively on the biological side — "find the structural problem and fix it." That strategy can be effective for acute injuries. For chronic pain, it frequently falls short.
A biopsychosocial approach matters because:
It explains why pain can persist long after tissues have healed
It opens the door to more effective, durable solutions
It gives patients a framework for understanding their own experience
It shifts focus from passive treatment to active recovery
Clinical guidelines now widely recommend multimodal, active care strategies for managing chronic pain rather than relying on passive treatments alone.
How Physical Therapy and Chiropractic Care Support This Model
A biopsychosocial approach does not mean doing less — it means doing the right things, at the right time, for the right reasons.
Physical Therapy
Physical therapy within this framework focuses on:
Gradual, confidence-building movement to rebuild trust in the body
Strengthening, endurance, and mobility work tailored to the individual
Retraining the nervous system's response to movement over time
Pain education to help patients understand what their symptoms mean
Restoring function for the activities that matter most in daily life
Movement, when dosed appropriately and progressed thoughtfully, is one of the most powerful tools available for calming a sensitized nervous system.
Why Education Is a Treatment in Itself
Understanding pain changes pain. When patients learn that movement is safe — and that pain does not always signal damage — fear tends to decrease, confidence tends to increase, and recovery becomes possible. Pain neuroscience education is not a soft add-on; it is a clinically supported component of effective chronic pain care.
Chiropractic Care
Chiropractic care complements physical therapy by:
Improving joint mobility and reducing movement restrictions
Providing sensory input that can modulate pain pathway activity
Supporting better movement patterns throughout the body
When integrated with education and active rehabilitation, manual therapy becomes a valuable component of a comprehensive, individualized pain care plan.
What You Can Do Starting Today
If chronic pain has been limiting your life, these practical steps can help interrupt the cycle:
Stay gently active. Avoid prolonged rest unless medically directed. Graded movement supports recovery.
Focus on progress, not perfection. Small, consistent improvements accumulate into meaningful change.
Address sleep and stress. Both have a direct, well-documented impact on pain sensitivity.
Reframe what pain signals mean. Pain is a protective warning system — not always a sign of ongoing damage.
Seek individualized care. Chronic pain is complex and personal. One-size-fits-all protocols rarely produce lasting results.
Ready to Experience the Living Well Approach?
Take the first step toward better movement and lasting relief.
Call 802-658-6092 or schedule your visit online to discover how chiropractic and physical therapy can work together to help you heal smarter and live well.
Schedule a physical therapy or chiropractic appointment today to restore mobility, relieve pain, and keep your body feeling strong all season.
Dr. Katherine Reardon - DPT
Katherine, a California native, completed her Doctorate in Physical Therapy from the University of the Pacific in 2019. Prior to that, she attended California State University Stanislaus, where she graduated Summa Cum Laude with a Bachelor of Arts in Kinesiology, concentrating on Health and Wellness Promotion. Katherine's experience as a physical therapist spans both outpatient and inpatient settings, where she developed a strong interest in adult orthopedic conditions and post-operative rehabilitation.
LEARN MORE→